We all know about the power of music to relieve stress and improve our mood. For older adults in hospice, music therapy can help control pain and improve their quality of life.
Sarah Michaels, music therapist at Tidewell Hospice, which provides hospice to patients’ homes and in specialty hospice houses, advocates for the benefits of music.
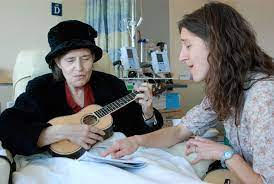
“I have been involved in music my whole life,” Michaels, who received her degree and board certification in music therapy from Florida State University, told McKnight’s Home Care Daily Pulse. “I started playing piano when I was in second grade, then joined band when I was in middle school. My initial thought of going into music therapy was that I wanted to work with kids. That kind of changed throughout the course of my studies. From there, that’s when I realized I liked working with older adults.”
The process
About two years ago, Michaels, who plays piano, clarinet and oboe, joined Tidewell Hospice. Before each session, Michaels begins by introducing herself and asking if the patient would like to hear some music. In home care settings, she usually gives a phone call before entering to give some context regarding who she is and what the session includes. From there, Michaels, who also receives referrals from social workers, finds a time to visit the patient.
In cases where a patient is nonverbal, Michaels said she tries to read facial cues.
“If they’re not giving me the best effect, I note that they don’t want to be bothered,” she added. “For the most part, people usually agree to the music. Then, my next question is ‘what kind of music do you like? I have country, I have religious, I have some jazz.’ Usually from there, after those few options, they’ll say ‘Oh, I really like country’ and from there I ask ‘Do you like older country or newer country’… and kind of go from there.”
Uses and benefits
The benefits of musictherapy are numerous, with some of the main ones including relaxation, helping to improve quality of life, pain management, socialization, family bonding and reminiscing, Michaels said.
“If they’re feeling tired, I try to keep my music soft and mellow,” Michaels said. “If they’re agitated, I try to find something a little more upbeat and then bring it down from there so they can calm down.”
During sessions, Michaels also often uses music therapy as a treatment add-on for pain management. She noted that having soothing music in the background, in addition to their prescribed medication, can be helpful.
“A lot of the time, I ask if they have any pain or how they’re feeling that day,” she said. “If they’re having a lot of pain, I may play something with a bit of a strum pattern and then go into a song with more of a picking pattern. They may be closing their eyes or taking slower breaths, especially if they are actively dying. Sometimes the breathing is more rapid, so I’ll definitely use music to help slow the breathing.”
When family is involved, and reminiscing is a part of sessions, Michaels will ask if the family members have a song in mind that they would like to hear. This leads to more conversation and socialization –– something that a lot of hospice patients lack in their lives.
“Sometimes they’ll pick a song that their family member would play all the time or sing to them, and that really creates nice conversation around the patient and among the family members,” Michaels remarked. “ So it’s another really special part of the music. It’s bringing about nice memories.”
Editor’s note: Home Sweet Home is a feature appearing Mondays in McKnight’s Home Care Daily Pulse. The story focuses on a heartwarming, entertaining or quirky happening affecting the world of home care. If you have a topic that might be worthy of the spotlight in Home Sweet Home, please email Liza Berger at [email protected].


